No more National Health Service

Sustainability and transformation plans are the Department of Health’s latest scheme to try to prevent the NHS slamming into the brick wall it’s accelerating towards. But are they going to work?
Words: Sid Ryan
Photo: Dean Ayotte (top image) and Mark Simmons Photography
Sustainability and transformation plans (STPs) are what’s in store for the NHS in the next five years. The term ‘STP’ is contentious because it’s not really a sustainable approach, nor really a plan – and although transformative, it’s not at all clear what the NHS is transforming into. The plans are being pushed through at light speed, during the NHS and local government’s biggest crisis in decades.
STPs, the government’s response to the NHS crisis, have been in development for the last year. Instead of the government taking control of the sector as a whole, the NHS is being broken up into 44 regional blocks, which are empowered to resolve their own problems in their own way. The Bristol, North Somerset and South Gloucester (BNSSG) region, made up of 15 NHS Trusts, CCGs and other health bodies, will get some limited powers to establish its own systems and set its own rules. As the ‘STP footprints’ start to diverge we’ll move away from a National Health Service and towards regional health services.
The programme for Bristol isn’t yet clear. NHS England, the Department of Health’s enforcer, has ordered that the plans be kept under lock and key for as long as possible. It was only after activist pressure and Freedom of Information requests by the Cable that the plans were released – and it was obvious why the government would prefer to keep them secret. The jumbled wish-list of projects generally falls into three categories: good ideas that make little overall difference, hopelessly optimistic ambitions, and bad excuses for cutting services.
What’s the plan?
The crux of the STP initiative is that if the NHS continues along its current trajectory, by 2020/21 there will be a deficit across the BNSSG region of £300 million per year. That shortfall will be in the form of either a gigantic budget crisis that needs to be bailed out by government, or more likely simply £300 million’s worth of healthcare that’s no longer provided.
To put that figure into context, Avon and Wiltshire Mental Health Partnership employs the equivalent of 3,300 full-time staff, serving a population of 1.8 million, with about 2,000 inpatients and 75,000 patients in the community. Abolishing the entire organisation would save £197 million – only two-thirds of the expected budget deficit – and would of course lead to all those untreated conditions worsening and requiring more care at greater expense.
There are no detailed proposals for how this budget gap will be closed. The STP project teams have identified £139m of cuts and ‘efficiencies’ under obscure headings, like the £35 million to be cut from North Bristol Trust’s “operational productivity” or an extra £10 million from University Hospitals Bristol seizing “commercial opportunities”. On top of these nebulous savings are a further £104 million of cuts that are yet to even be identified.
More problematic is that many of the savings programmes supposed to be carried out need a significant amount of investment in new technologies and new working teams. The savings these plans are supposed to generate are booked, but their delivery is far from certain. The “sustainable transformation fund”, a one-off £61 million block of funds from government supposed to support the transition, is mostly being earmarked for shoring up pre-existing budget deficits rather than addressing the root causes.
When the three local councils in the BNSSG region met to scrutinise the plans, not one councillor spoke in favour of the STP. The most common concern was the concurrent social care crisis. Lockleaze councillor Gill Kirk said: “The council has already made big savings in social care but still have a shortfall and there’s no new money coming. The chancellor is content to say that there will be some money for social care in 2020. The problem is, what are we going to do until then? The needs of those people are urgent and there isn’t any funding.”
Where are we going?
Seeking to avoid legal challenges against the STP, instead of concrete and credible proposals the plans are based around ‘frameworks’ and ‘principles’. The problem is that no-one could ever object to the principle – it’s the execution that causes concern, and the Department of Health’s track record on reforming the NHS that exacerbates it.
‘Care closer to home’ is one such idea. In principle it looks to help patients manage their own long-term conditions and give them some independence from the health system. ‘Managing demand’ is supposed to reduce the number of contacts with GPs and community care services by 15%, reduce hospital admissions by 30% for some conditions and cut the average length of a stay in hospital by 20%. Reading between the lines you get the impression that patients are being asked to look after themselves because the NHS no longer can.
“This looks like rationing of healthcare,” says Mike Campbell, a member of campaign group Protect Our NHS. “Even if there was enough money to set this new system up, which there isn’t, it’s going to lead to more people falling through the cracks and not getting the care they need. Self-care might make sense for some, but it’s vulnerable people who’ll suffer.”
The other concern for health campaigners is the spectre of privatisation. All STP areas are being encouraged to follow an ‘Accountable Care Organisation’ model, an import from the US health system. Effectively a single umbrella organisation to provide care for an area, it is funded a fixed amount per person in its area. Not only does this encourage ‘care to fit your budget’ rather than your needs, it could lead to the introduction of top-up fees and co-payments (fixed fees paid each time a medical service is accessed).
The other danger, though less so in a big city like Bristol, is that one or more of the 44 STP areas collapses into financial ruin only to be bought up by a private firm. Over the previous 15 years private providers have been increasing the scale of their holdings, first targeting specific treatments such as cataract surgery, then onto whole bundles of services such as Virgin Care recently taking over community health and care in Bath. Now the NHS offers the prospect of a regional monopoly over the entire health and social care system.
Push back
The STP is supposed to pull the NHS back from the brink, and yet the planning documents admit that we need change “at a scale not previously seen” with a “limited evidence base that exists for achieving” that change. In ‘bureaucratese’, that’s a pretty clear message that the STP is a road to ruin, and yet it will continue anyway unless it is challenged.
Even the supposed cheerleaders for the sustainability and transformation plan, the local health service bosses responsible for developing and implementing it, are finding it hard to defend. Robert Woolley, chief executive of University Hospitals Bristol Trust, said it was “inappropriate” for the plans to be developed with so little input from patients, the public and the council. He emphasised that he and his colleagues were being asked by their “lords and masters” to develop the plans in whatever “spare time” they had left over after running some of the largest NHS Trusts in the country.
The next few months will be critical and the stakes couldn’t be much higher. Although there is a half-hearted attempt to fulfil the legal duty to consult with members of the public, remember that there’s only one relevant question here: is healthcare going to get better or worse? So far there’s not much evidence to suggest the former. Which means we’ve got some work to do.




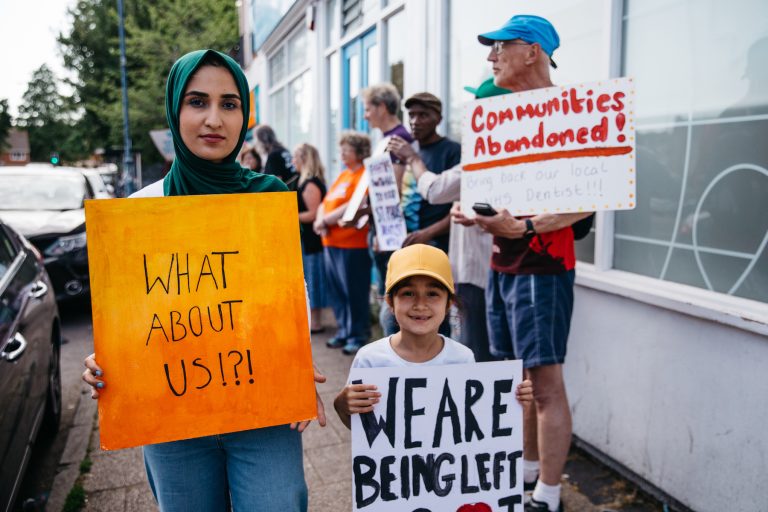








Report a comment. Comments are moderated according to our Comment Policy.